Jason D. Lazarus, J.D., LL.M., CSSC, MSCC
If you are confused by the myriad of government benefit programs that many clients receive as a result of being a personal injury victim, don’t worry as you are not alone. Most times personal injury victims are not sure either about the benefits they receive and can confuse the different programs. This is not surprising as the acronyms for the programs are similar and governed by the same or similar government agencies. For example, a disabled client might get Supplemental Security Income (SSI) or Social Security Disability Insurance (SSDI). While similar in terms of who qualifies and both provided by the Social Security Administration, how you qualify for each are vastly different. Another example is Medicare and Medicaid. Both involve the same agency, Centers for Medicare & Medicaid Services; however, Medicare is an entitlement that is administered entirely federally while Medicaid is income/asset sensitive and is administered mostly at the state level. All of these benefits have unique issues and different planning solutions must be employed.
The goal of this post is to clarify the information and make it easy to understand.
The following chart is a good starting point to understanding public benefits:
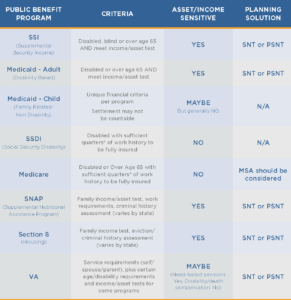
To understand the table, you should know a few acronyms.
- While the SS in SSDI and SSI stand for different things, you can use these first two letters as an easy way to remember that both are offered by the Social Security Administration.
- VA stands for Veterans Administration.
- SNT and PSNT stand for Special Needs Trust and Pooled Special Needs Trust, respectively.
- MSA stands for Medicare Set-Aside.
- There is no such thing as a Medicaid Set-Aside and there are many differences between how SNTs and MSAs operate.
Many times there is confusion about the proper planning solutions a client might need but by the time you are done reading this post, it should be much clearer.
Understanding Public Assistance Programs
There are two primary public benefit programs that are available to those who are injured and disabled. The first is the Medicaid program and the intertwined Supplemental Security Income benefit (“SSI”). The second is the Medicare program and the related Social Security Disability Income/Retirement benefit (“SSDI”). Both programs can be adversely impacted by an injury victim’s receipt of a personal injury recovery. Understanding the basics of these programs and their differences is imperative to protecting the client’s eligibility for these benefits.
Medicaid and Supplemental Security Income (hereinafter SSI) are income and asset sensitive public benefits that require special planning to preserve. In many states, one dollar of SSI benefits automatically provides Medicaid coverage. This is very important, as it is imperative in most situations to preserve some level of SSI benefits if Medicaid coverage is needed in the future. SSI is a cash assistance program administered by the Social Security Administration. It provides financial assistance to needy, aged, blind, or disabled individuals. To receive SSI, the individual must be aged (sixty-five or older), blind or disabled, and be a U.S. citizen. The recipient must also meet the financial eligibility requirements. Medicaid provides basic health care coverage for those who cannot afford it. It is a state and federally funded program run differently in each state. Eligibility requirements and services available vary by state. Medicaid can be used to supplement Medicare coverage if the client is eligible for both programs (“dual eligible”). For example, Medicaid can pay for prescription drugs as well as Medicare co-payments or deductibles. Because Medicaid and SSI are income and asset sensitive, creation of a special needs trust and/or ABLE account may be necessary, which is discussed in greater detail below.
Some other benefits that are needs-based are Food Stamps, Supplemental Nutritional Assistance Program (SNAP), Section 8 (housing) and some Veterans Administration benefits (non-service connected). Since these benefits are not necessarily protected by the use of traditional planning tools like an SNT, these are more complex to protect. In many instances, it makes more sense to lose these benefits and allow an SNT to pay for these needs or use an ABLE account to pay for those types of expenses. What complicates the payment of some of these types of benefits is the SSI restriction on paying for food & shelter. That is where an ABLE account can come in handy since it is exempt from such rules (but there are limitations on who can create an ABLE account). There are also some other financial-based planning techniques to try and preserve these benefits, but it does vary by program so consulting with an expert is imperative to help with the planning.
Medicare and Social Security Disability Income (hereinafter SSDI) benefits are an entitlement and are not income or asset sensitive. Clients who meet Social Security’s definition of disability and have paid in enough quarters into the system can receive disability benefits without regard to their financial situation. The SSDI benefit program is funded by the workforce’s contribution into FICA (social security) or self-employment taxes. Workers earn credits based on their work history and a worker must have enough credits to get SSDI benefits should they become disabled. Medicare is a federal health insurance program. Medicare entitlement commences at age 65 or two years after becoming disabled under Social Security’s definition of disability. Medicare coverage is available again without regard to the injury victim’s financial situation. Accordingly, a special needs trust is not necessary to protect eligibility for these benefits. However, the MSP may necessitate the use of a Medicare Set Aside discussed in greater detail below.
Planning Tools for Public Benefit Recipients
Medicaid/SSI
For those that receive needs-based public benefits such as SSI/Medicaid, there are planning devices that can be utilized to preserve eligibility for disabled injury victims. A special needs trust can be created to hold the recovery and preserve public benefit eligibility since assets held within a special needs trust are not a countable resource for purposes of Medicaid or SSI eligibility. The creation of a special needs trusts is authorized by Federal law. Trusts commonly referred to as (d)(4)(a) special needs trusts, named after the Federal code section which authorizes their creation, are for those under the age of 65. Another type of trust is authorized under by Federal law with no age restriction and it is called a pooled trust, commonly referred to as a (d)(4)(c) trust.
The 1396p provisions in the United States Code governs the creation and requirements for such trusts. First and foremost, a client must be disabled in order to create an SNT. There are two primary types of trusts that may be created to hold a personal injury recovery each with its own requirements and restrictions. First is the (d)(4)(A) special needs trust which can be established only for those who are disabled and are under age 65. This trust is established with the personal injury victim’s recovery and is established for the victim’s own benefit. It can be established by the injury victim themselves, a parent, grandparent, guardian or court order. Second is a (d)(4)(C) trust typically called a pooled trust that may be established with the disabled victim’s funds without regard to age. A pooled trust can be established by the injury victim and others just like a (d)(4)(A). Both trusts operate identically and provide for the special needs of a client. The primary restrictions on use of the money are that it must be for the sole benefit of the trust beneficiary, the trust cannot provide cash and it cannot be used for food or shelter (for those that receive SSI). Other than that, it can provide for nearly anything that improves the trust beneficiary’s quality of life.
Oftentimes, an ABLE account can be used in conjunction with an SNT or instead of an SNT. An ABLE account is a tax-advantaged savings account for disabled individuals. An ABLE account can pay for any “qualified disability expense” which is quite broad and does not impose restrictions on food/shelter payments. An ABLE account can only be established by someone who is disabled and whose onset of disability occurred prior to turning 26 years of age. An ABLE account can only be funded up to a maximum amount of $15,000 annually and only the first $100,000 in funding is exempt from the SSI asset/resource test. ABLE accounts remain a limited option and only makes sense in certain circumstances.
Medicare/SSDI
A client who is a current Medicare beneficiary or reasonably expected to become one within 30 months should concern every trial lawyer because of the implications of the Medicare Secondary Payer Act (“MSP”). Since under the MSP Medicare is not supposed to pay for future medical expenses covered by a liability or Workers’ Compensation settlement, judgment or award, CMS recommends that injury victims set aside a sufficient amount to cover future medical expenses that are Medicare covered. CMS’ recommended way to protect an injury victim’s future Medicare benefit eligibility is establishment of a Medicare Set-Aside (“MSA”) to pay for injury-related care until exhaustion.
In certain cases, a Medicare Set-Aside may be advisable in order to preserve future eligibility for Medicare coverage. A Medicare Set-Aside allows an injury victim to preserve Medicare benefits by setting aside a portion of the settlement money in a segregated account to pay for future Medicare covered healthcare. The funds in the set-aside can only be used for Medicare covered expenses for the client’s injury-related care. Once the set-aside account is exhausted, the client gets full Medicare coverage without Medicare ever looking to their remaining settlement dollars to provide for any Medicare covered health care. In certain circumstances, Medicare approves the amount to be set aside in writing and agrees to be responsible for all future expenses once the set-aside funds are depleted.
The problem is that MSAs are not required by a federal statute even in Workers’ Compensation cases where they are commonplace. There are no regulations, at this time, related to MSAs either. Instead, CMS has intricate “guidelines” and “FAQs” on their website for nearly every aspect of set-asides from submission to administration. There are only limited guidelines for liability settlements involving Medicare beneficiaries. While there is no legal requirement that an MSA be created, the failure to do so may result in Medicare refusing to pay for future medical expenses related to the injury until the entire settlement is exhausted. There has been a slow progression towards a CMS “policy” of creating set-asides in liability settlements over the last seven years as a result of the Medicare Medicaid SCHIP Extension Act’s passage. All of the uncertainty surrounding set-asides creates a difficult situation for Medicare beneficiary-injury victims and contingent liability for legal practitioners as well as other parties involved in litigation involving Medicare beneficiaries. There do appear to be regulations on the horizon for set-asides based upon Medicare’s renewed focus on it for 2019. For the time being, a set-aside analysis should be considered for settlements or judgments involving current Medicare beneficiaries.
Dual Eligibility – Medicare & Medicaid
Clients who receive both Medicaid and Medicare require extra planning to preserve all government benefits. If it is determined that a Medicare Set-Aside is appropriate, it raises some issues with continued Medicaid eligibility. A Medicare Set-Aside account is considered an available resource for purposes of needs-based benefits such as SSI/Medicaid. If the Medicare Set-Aside account is not set up inside a Special Need Trust, the client will lose Medicaid/SSI eligibility. Therefore, in order for someone with dual eligibility to maintain their Medicaid/SSI benefits the MSA must be put inside a Special Needs Trust. In this instance, you would have a hybrid trust which addresses both Medicaid and Medicare. It is a complicated planning tool but one that is essential when you have a client with dual eligibility.
Conclusion – Protect Your Client, Protect Your Firm
Disabled clients need counseling at settlement given the likelihood they will be receiving some type of government benefits. To prevent being exposed to a malpractice cause of action, the personal injury practitioner should understand the types of public benefits that a disabled client may be eligible for and techniques that are available to preserve those benefits. Having this knowledge will help the lawyer identify disabled clients they may want to refer for further consultation with other experts.
When a settlement involves the protection of public benefits or settlement assets, outside counsel is typically retained to assist with the trust devices commonly used to protect the client. Lawyers who are well-versed in “settlement law” or “settlement planning” can be found and relied upon to assist with these difficult and complicated issues. The legal fees for creation of the trusts to protect the settlement monies or public benefit eligibility are normally paid for out of the injury victim’s recovery.
Companies such as Synergy deal with these issues on a daily basis. Having a consultant familiar with the planning issues and who has access to the right solutions is imperative. This is where Synergy’s settlement consulting/planning team really shines and can be an invaluable member of your settlement team. Having the knowledge of the public benefit programs along with issues such as Affordable Care Act coverage and options is a non-negotiable these days given the complex settlement landscape.
To learn more watch representing clients with government benefits watch our educational video below.




